
The COVID-AM blog is a partnership between the UMI 3157 iGLOBES and the Institut des Amériques, coordinated by François-Michel Le Tourneau, Deputy Director and Marion Magnan, researcher at the Institute. About the blog.
the Political Economy of social protection in colombia: COVID-19 as an indicator
July 1, 2020

by Thibaud Deguilhem, Professor in Economy at Université de Paris (LADYSS). Member of the Scientific Committee of the Institut des Amériques 2021 Conference
The World Health Organization is considering Latin American as the new world epicenter of the virus since May 22.
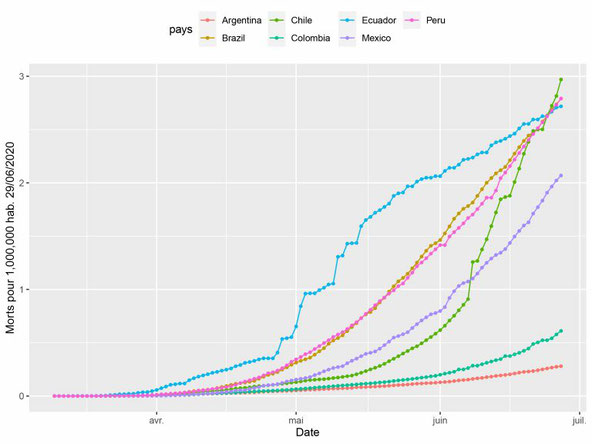
Seeming to be in better shape than its neighbors from the data given at the international level (Figure 1), Colombia is however no exception to the rule and has been confronting the brutal pandemic shock for over three months now.

At first, the health crisis in the country almost immediately stretched hospital capacity, already very limited before the pandemic (1.7 hospital beds for 1000 inhabitants and only 1.3 nurses for 1000 inhabitants in 2018). Confronted with the structural weakness of the health system and the regional differences in the spread of the virus in the country, the OECD, which Colombia has officially joined since April 28, called for a more decentralized management of the crisis. Yet, far from the adjusted response promised by the successive decentralization policies applied in the country, it's mainly disorganization that is prevailing. Vacillating between the inertia of the government's intervention and the determination of municipalities,
particularly Bogota, the various administrative agencies are having a difficult time intervening in an appropriate fashion and providing the needed means of protection and subsistance. This phenomena is particularly noticeable in vulnerable urban areas of the capital. Whole sections have at times been totally cut off from the rest of the city under total lockdown, such as Kennedy, while others, more vulnerable, are facing police pressure and the programmed demolition of informal housing in Ciudad Bolivar south of Bogota.
Put in place to quickly deal with the urgency of the health crisis, the lockdown measures ajusted according to the geographic zone have had, at a later stage, social-economic repercussions, the breadth of which is still far from being recognized or even estimated. Despite this significant uncertainty on the long-term effects, the consequences are already numerous and cumulative. The contraction of the domestic supply and demand, the sudden stop in international exchanges and the fall of the price of raw materials for a Colombian capitalist economy based on the export of natural resources, such as oil, makes for an explosive situation leading to the massive elimination of jobs (close to six million at the national level), and to calling into question the fragile results obtained in the fight against poverty these past fifteen years. Direct repercussions from this shock wave, requests for emergency help are more and more pressing when faced with the loss of revenue and hunger which cruelly resurfaces in the heart of the capital.

In the end, the institutional failures are being uncovered day after day, creating in Colombia, as in other places, an unbearable debate around deciding between the short-term health "costs" and social-economic "costs", notably pushing the government to defy its own health measures by putting in place a day without taxes ("día sin IVA") in the middle of the lockdown. Despite these interventions, more perilous for the health of the Colombians and counter-productive for the government's resources than effective for a hypothetical economic boost, this crisis will be long term and calls for reconsidering both the long-term social "costs" and the perspective of a new "lost decade" in Latin America are more and more widespread (McKee et Stugler 2020[1]). Yet, though many of the Latin-American experts agree on the need to take another look at the weaknesses of the social protection at a regional level, few backtrack and rethink the failure of the social compromises that were made in the past thirty years, especially in Colombia.
During the 1990s and the crafting of the second Washington consensus, the government that had introduced a public social security with the law 100 of 1993, following the constitutional reform of 1991, quickly considered restricting its scope, consistent with the objective of "good governance", rationalizing public expenses (Salama et al. 2005[2]). In the 2000s, this paradigm is again reinforced and now it's the slow and progressive substitution of this new social security that is then considered, articulating between the fight against poverty and the financialization of the welfare market. At the base of the social structure, the cash-transfer programs such as the famous "familias en acción" in Colombia focus on "pro-poor" targeting rewriting social welfare, for the poor and vulnerable households, in a narrower field of assistance. At the top of the social-economic hierarchy, public insurance mechanisms are little by little put aside for the expansion of the financiarization of welfare with a rate reduction for those who are better off. Far from strengthening the capabilities of the government and the vulnerable households, this deconstruction that is historic, institutional and paradigmatic in fact creates a social system that is fragile, fragmented and segmented.
So, on the eve of the pandemic blow, though a large majority of Colombian households had minimal coverage via a mixed system (contributions or subsidies, relics from the law 100 of 1993), about 10% of them still had nothing and for the others, coverage was often limited to basic care and meant low quality care. For the many other social risks (unemployment and old age in particular), households are based individually on their own social status, enabling them to benefit from cash-transfer programs, under certain conditions. For a small well-off minority, the private insurance sector enables them to benefit from the same type of coverage as that of the countries with a higher level of human development. A consequence of this structural fragmentation, the inequalities of access to the means of preventing risks are high in the country, and are added to the many other types of disparities, between urban and rural zones, between men and women, and toward indigenous populations.

Another consequence of this fragmented system, the cost of coverage is often prohibitive for households, many of which give up on protecting themselves as seen in the research in the region (Koch et al. 2017[3]). The poorest and most vulnerable then have to rely on local solidarities for their coverage, that are fragile and are jeopardized when there are covariant blows, as what was painfully observed particularly in Bogota with the impact of the lockdown on the weakening intracommunity capabilities. Despite the relative universal healthcare model and its place in the institutional organization specific to the type of capitalism in Colombia, the social compromise, stabilized until now, forces many households in the "vulnerability trap" vicious circle that maintains them in socially fragile situations. Solely dependent on salaries from low quality jobs, they are all the more exposed to risks against which they have none or little coverage (Deguilhem et Vernot Lopez 2020[4]).
Ultimately, the combination of structural fragmentation of the protection mechanisms and the blow of the pandemic requires that the social situation be reevaluated beyond the tight prism of emergency aide in order to reestablish a social-developmental compromise, in Colombia in particular, and in Latin America as a whole (see how this issue is examined in Peru). Though the outcome of this multiple crisis today is uncertain, getting back to the notion of social protection as a "set of mediation between economic, political and domestic order", which would help (re)include the most divided types of protection, from family and community solidarities to plans that were surrendered to the markets, (Lautier et al. 1995[5]), should be considered an even more pressing matter than the economic recovery of a model both deficient and fragile. "(Re)-shaping society" after the blow and preventing future social-environmental upsets, already present in a country etched with inequalities, will require reconfiguring a national compromise in favor of unified social protection, widespread and reinstutionalized.
[1] McKee, M., & Stuckler, D. (2020). If the world fails to protect the economy, COVID-19 will damage health not just now but also in the future. Nature Medicine. April 9, 2020.
[2] Salama P., Marques-Pereira J., Lautier B., Le Bonniec Y., Rodriguez Salazar O. & Giraldo C. (2005). Sistemas de protección social: entre la volatilidad económica y la vulnerabilidad social. Bogota: Universidad Nacional de Colombia.
[3] Koch, K. J., Cid Pedraza, C., & Schmid, A. (2017). Out-of-pocket expenditure and financial protection in the Chilean health care system-A systematic review. Health Policy, 121(5), 481–494.
[4] Deguilhem T. & Vernot Lopez M. (2020). De la informalidad a la calidad del empleo: ¿cuáles son los desafíos para américa latina? Foreign Affairs Latinoamerica, 20(1), 44–53.
[5] Lautier, B., Belorgey, J. & Holland, S. (1995). L’État et le social. Dans: Bruno Théret éd., L’État, la finance et le social (pp. 483-533). Paris: La Découverte.
Thibaud Deguilhem is a Professor in Economy at Université de Paris and researcher in the lab Dynamique Sociales et Recomposition des Espaces (LADYSS) UMR 7533. Member of the Scientific Committee of the 2021 Institut des Amériques conference. His research mainly focuses on the inequalities in the job market, employment institutions, living conditions of households and healthcare policies in Latin America and Africa. His personal website and published works accessible on ResearchGate.
